
In the beginning days of what would ultimately be the SARS-CoV-2 pandemic, the United States made a series of critical missteps in preparation for the onslaught of the virus. A state-by-state approach to combat a highly contagious infectious disease – that did not claim residency to a specific commonwealth – was destined for failure. Before we could blink, hospitals in high-density regions like New York City looked like a scene straight out of a horror movie. As I write this, the U.S. has seen two large surges of SARS-CoV-2 and leads the world in confirmed infections and deaths attributed to the virus.
As a virologist, I wish I could say that we have learned from our mistakes and implemented sound policy and uniform public health guardrails to combat the virus; however, that has not been the case. In the past few weeks, many of us in the infectious diseases sphere have seen very concerning trends foreboding a massive wave of COVID-19 cases in the coming months. The Institute for Health Metrics and Evaluation (known as the IHME), one of the most cited sources for epidemiological data and predictions during the pandemic, recently upped their expected death total to more than 400,000 by January 1st, 2021. While I believe this is on the higher range of what we should reasonably expect, many physicians and scientists anticipate a new surge in the coming months.
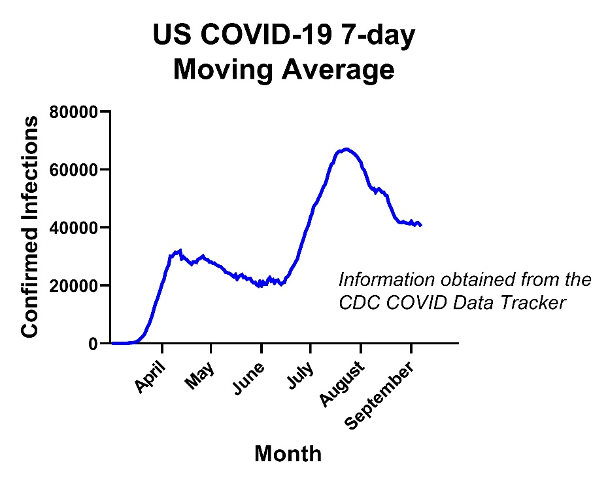
There are several factors at play here, and I’ll briefly attempt to go over a few of them. The first, most-apparent flashing red light is that we have yet to get the virus under control. As a nation, we seem to have hit a hard floor of ~35,000 – 40,000 new confirmed infections per day. Recall that the U.S. also hit a floor of ~20,000 new confirmed cases per day in late May-early June. Similar to then, what we have now is sustained community transmission of SARS-CoV-2 throughout the U.S. This base level of spread can prime an environment for a rapid burst of infections at the local level, translating into a more wide-scale outbreak.
A great example of this is the Sturgis Motorcycle Rally that took place in South Dakota from August 7th – 16th. An estimated 460,000 individuals attended this rally, which was complete with concerts, bike shows, and luncheons crammed into a city with less than 7,000 locals. If we were to arbitrarily assume that a mere 1% of attendees were infected with the virus at the time, then 4,600 people brought it with them. Researchers at San Diego State University estimated that this rally might have resulted in over 250,000 new infections with SARS-CoV-2. Subsequent analyses have questioned how accurate this estimate might be. Still, there should be no doubt that sustained community spread throughout the U.S. allowed the virus to be brought to the rally and spread. Unlike February and March, the virus is not localized to a handful of states and densely-populated metropolitan areas; instead, it is endemic, meaning that it is now interwoven into communities throughout the nation and poised to cause major rapid outbreaks.
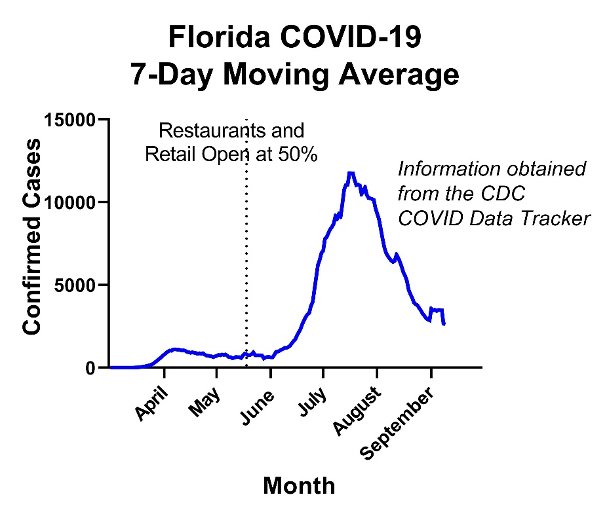
The second major cause for concern that we have seen is an increase in transmission of SARS-CoV-2 among young adults. This was the case during the first resurgence of SARS-CoV-2 seen in June/July. Several states barreled into premature reopening strategies without demonstrating sustained decreases in the virus’s transmission rate. The first patients to become infected were young adults returning to work. Although it is a true statement that young adults tend to have better clinical outcomes compared to older adults, their ability to transmit the virus can be just as effective. Therefore when states moved to open prematurely, the young and working-age adults who spent their working-hours in confined areas contracted SARS-CoV-2, and then community spread ensued. Case-in-point for this would be Florida, which moved to reopen retail and restaurants on May 18th, and a predictable disaster followed.
Fast forward a few months to the present day: It’s difficult to turn on your local news without hearing that a local school or university had to move into remote operations due to spikes in students. The University of North Carolina opened during the first week of August and subsequently forced to move to remote learning by the end of the month. Rather than UNC being viewed as the “canary in the coal mine,” other institutions attempted to re-open their campuses to have the same outcome. Mixed messaging about COVID-19 puts young adults at risk. Moreover, it also increases the chances that they transmit the virus to higher-risk populations.
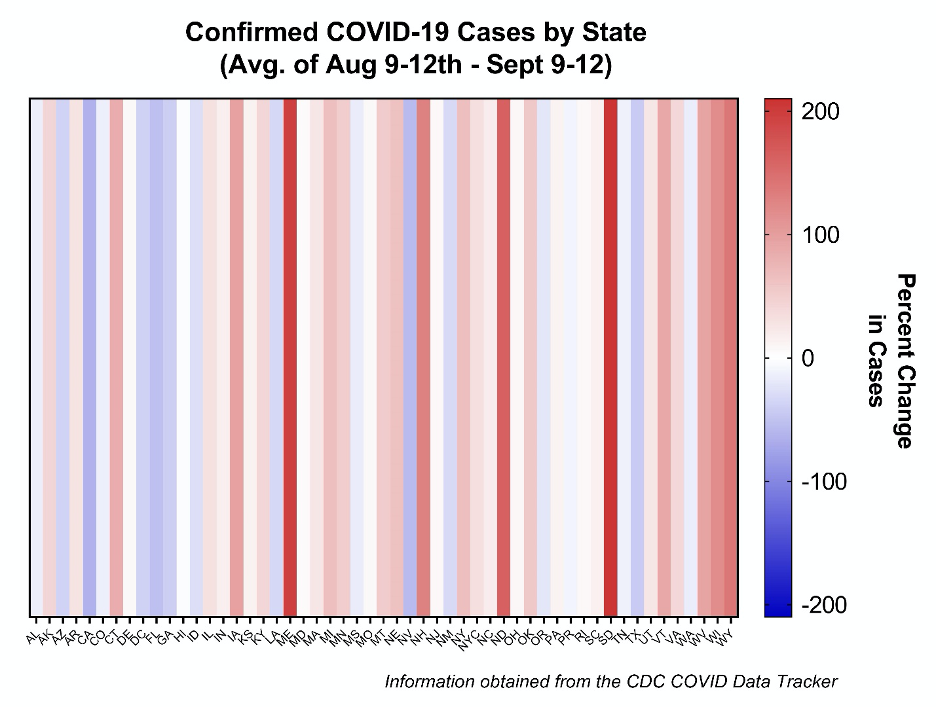
A third major cause of concern for a fall surge of SARS-CoV-2 is the patchwork plan to combat this pandemic. It’s the hallmark of our failure to contain it since March. It’s important to note that the summer surge of SARS-CoV-2 was not equally felt throughout the U.S – it was localized to the sunbelt states. Similarly, the first wave of COVID-19 cases in the U.S. was primarily in the northeast and parts of the Midwest. In a month-by-month comparison, you can see below that many states are seeing massive spikes of cases. For example, South Dakota has seen a 206% increase in cases, mainly attributed to the Sturgis Bike Rally. This graph does not account for population density, so the 64% decrease in cases in the state of California can more than compensate for the large spikes seen in states like S.D., ND, and W.V. However, we would like to see a more uniform decrease in cases throughout the U.S.
Instead, you can see several deep red patches – indicating a high percentage increases in transmission – and a smattering of light blue, showing decreased percent transmission. Until we can get to a point where the entire graph is various shades of blue, we risk local healthcare infrastructures being overrun, translating into an increase in infection fatality rates of COVID-19. This fact is especially true for America’s rural regions with fewer resources needed to treat cases such as ICU beds and ventilators.
Another primary concern that we have seen is the American public’s mobility in recent weeks, combined with the seasonal changes in behavior that we will see in the coming months. The re-opening of schools, universities, and businesses that resulted in spikes in cases can be rapidly compounded by the fact that the newly infected patients (mostly young adults) are more mobile. So when the school or business is forced to close down, the infected young adults can then transmit the virus to their local community. This fact is particularly problematic since the spread of SARS-CoV-2 can occur before the onset of symptoms.
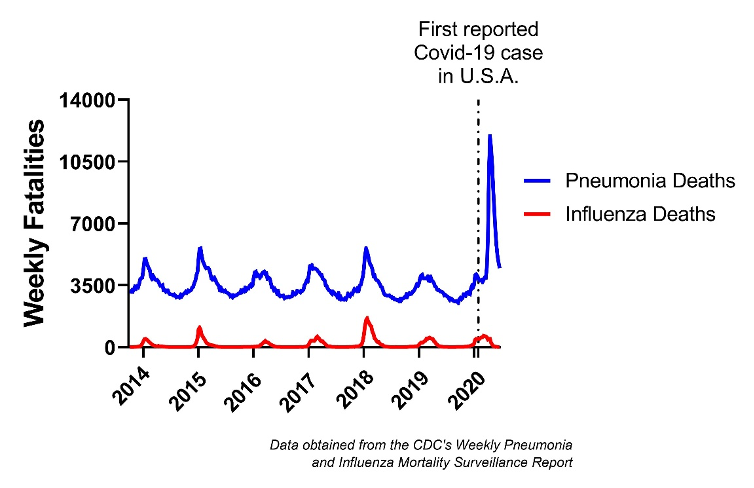
The second component of this concern is the changes in human behavior during the fall and winter. There tends to be much more activity indoors as the weather cools, allowing respiratory pathogens to spread more efficiently (along with some other factors that I won’t get into here). Our knowledge of transmission of the virus has increased substantially since the spring. It has become clear that indoor activities involving high-density crowds are the primary source of super-spreading events. Events like choir practices, church gatherings, and bar patronage have shown that SARS-CoV-2 can spread to dozens of people from a single infected person. It can accomplish this by hitching a ride on exhaled respiratory droplets and aerosols, allowing the virus to linger in the air like a cloud for minutes without proper ventilation. Loud speaking, singing, and chanting have been shown to increase exhaled droplets and aerosols; therefore, places like choir practices or indoor locker rooms are veritable buffets for this virus. It is not surprising that several college football games had to be canceled on week one, and already several games canceled for week two, due to COVID-19 clusters among student-athletes and coaches. Undoubtedly there will be more as teams travel and person-to-person contacts increase throughout the fall. If SARS-CoV-2 tracks are similar to the influenza virus, we could be in for a deadly next six months.
In sum, there is still far too much transmission of COVID-19. Many of the new cases are represented heavily in young adults, who are more mobile than other age demographics and rapidly spread the virus at the local and state levels. As we transition into the fall when indoor activities increase, the potential for super-spreading events increases. Each of these trends that I’ve gone over in this article is additive. By themselves, virus spread would be limited, but they are a row of dominoes ready to fall when combined. The only question is whether we have pushed that first one over already…
______________________________________________________________________________________________________________________






