The world received fantastic news in early November – the vaccines are on the way. In record time, we have produced two candidates with higher efficacy rates than the 70% called for by the National Institutes of Health. Pfizer and Moderna have started getting approval for the use of their vaccine candidates, and many jurisdictions are predicting they can begin vaccinating citizens as early as mid-December. The UK-based AstraZeneca candidate also reported a high efficacy rate this week, and countries like India and the UK anticipate starting deployment in January. Canadian authorities are enlisting military planning and dispersion experts. With these revelations, we need to discuss several issues with vaccines while deploying this undoubtedly crucial pillar of our effort to returning to a recognizable world.
Before launching into the discussion, it is worth highlighting that vaccines will not singlehandedly change our world overnight, but they are a giant leap towards restoring a semblance of normalcy. We all want to go back to going to work and school, visiting loved ones, attending concerts and sporting events, and socializing in general without fear of getting infected or unknowingly infecting others. As a person with a disability living in a care facility, I have not touched my children since March 2nd. I still see them, but every scrupulously scheduled visit is conducted behind Plexiglass dividers. Let’s fix that.
What did we achieve?
Governments all over the World have agreed to buy hundreds of millions of doses of vaccines from hundreds of candidates currently in trial or striving for approval. There are a staggering 321 vaccines against SARS-CoV-2 in some stage of development at the time of writing, with 43 in Phase I or II human trials and twelve in Phase III. More advance every day.
Two are already in use overseas: A Chinese vaccine was deployed to military and key infrastructure personnel starting in July, and another was deployed in Russia in August.
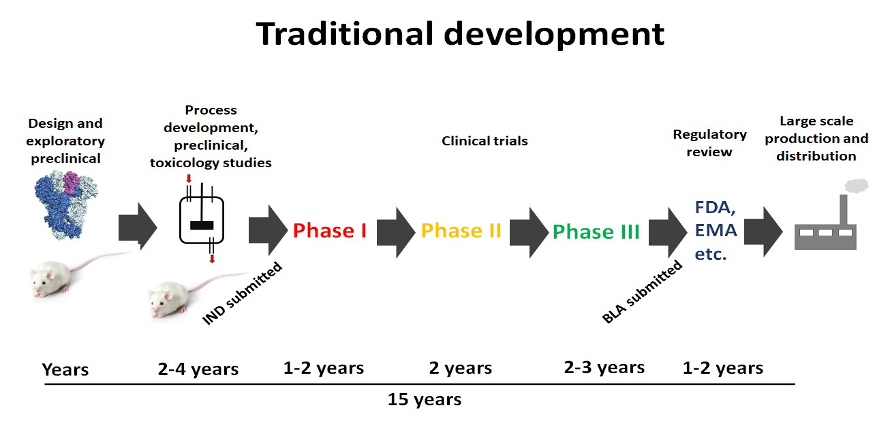
The fact that we already have this many promising vaccine candidates is staggering. The standard process of development takes an average of 10-15 years.
We have shattered the previous record for vaccine development. The quickest vaccine developed to date was the Mumps vaccine, which took four years from preclinical research to deployment. We are poised to grant Emergency Authorization in December and start vaccinating essential workers and high-risk groups an astounding 11 months after discovering the genome.
What are vaccines supposed to do anyway?
When the body is exposed to a new pathogen – such as a virus, bacterium, fungus, etc. – a non-specific system called the ‘innate immune system’ begins immediately. A short time after infection, the ‘adaptive immune system’ is turned on to identify the specific intruder and prompt white blood cells to generate immunoglobulin proteins (ie. antibodies) that attack the invader. Other cell types are primed to find and attack infected cells with proteins and enzymes independent of antibodies.
The most ingenious aspect of the system is that the body maintains a memory bank of which cells and antibodies we have used before. If that same challenge returns, the body can recognize it and rapidly mobilize an army of defenders tailored specifically to neutralize and destroy that invader – quickly enough that the invader doesn’t even have a chance to get a toehold and start reproducing.
Vaccines mimic that natural process by getting the body to put a new entry into the library of recognized enemies without having to fight off an infection.
The process works. Measles is exceedingly rare in modern times – thanks to vaccines. Smallpox killed millions of people worldwide until 1977. That virus no longer exists (except frozen in a handful of labs). Cervical cancer is increasingly rare due to HPV vaccination, such that the need for a Pap Smear will likely be eliminated in the next couple of decades.
It would seem intuitive that such an effective intervention would be broadly accepted, but that isn’t the case.
Do we even need vaccines?
Once enough people in a population are immune to catching and transmitting a disease, the pathogen cannot find a new susceptible host. It stops spreading freely – a much-discussed concept called “herd immunity.”
This phenomenon can be achieved through vaccination but also – theoretically – through natural infection. This is the route suggested in the Great Barrington Declaration and advocated by some in the US coronavirus Task Force. They propose that protecting the highest risk people while simultaneously allowing the virus to spread in the young & healthy will speed the attainment of herd immunity. In theory, a vaccine would not even be necessary to achieve it. Critics question the ethics of allowing people to become infected that don’t need to be – mainly where long-term effects are still unknown.
Who gets the vaccines?
The principle of “Vaccine Nationalism” is another controversial issue, recently challenged convincingly by German President Frank-Walter Steinmeier. The idea is that countries that fund development – or do the research in domestic labs – should be first in line vaccinating their citizens.
Most of the world signed onto an UN-sponsored vaccine agreement that committed the first 20% of vaccines to be divided among all countries to immunize their key personnel (e.g., doctors & nurses) and highest risk citizens. The remaining 80% would be strategically distributed to best combat disease transmission and mutation risk – wherever that may be. Participants at the recent G20 Summit recommitted to the strategy.
The United States notably did not sign-on. Under the Trump administration, the official policy is to vaccinate all Americans first, then help elsewhere.
A recent study estimated taking a vaccine nationalism position (those who can afford it first) will result in 28% more unnecessary deaths worldwide. I also question the wisdom of allowing the virus to spread outside of borders – the reintroduction of a potentially mutated virus seems inevitable.
Will we take them?
You have likely heard the maxim “Vaccines don’t stop disease…vaccination does.” The intervention is useless if no-one will use it. Surveys of vaccine acceptability suggest the majority of the world’s population would accept a vaccine recommended by the government – ranging from 90% in China down to 55% in Russia. But acceptance is improving. In Canada, a recent poll showed 69% would take a vaccine. In the United States, it’s 58%. More alarmingly, however, 42% said they would never take one.
Estimates vary of how many people will need to take an effective vaccine to halt transmission vary. Most authorities suggest a 60-80% uptake of a 50% efficacious vaccine – through The University of Washington calculates as low as 43% deployment may be enough. With the reported efficacy of Pfizer and Moderna’s candidates, we could conceivably get away with even fewer.
It should be noted that “anti-vax” is a different phenomenon from vaccine hesitancy. Anti-vax proponents feel that vaccines pose a distinct threat and will under no circumstances allow one to be put into them or their children. Reluctance to take a vaccine is a rational response to concerns about rushed development, questionable oversight, untested mechanisms, or safety. Making that Risk-Benefit calculation is not an Anti-Vaxx decision based on misinformation or reflexive fear.
Can we make people take them?
We are undoubtedly headed towards a monumental societal battle. The ‘social contract’ obligations we have to our communities, and personal freedoms will be in an epic conflict. It will likely be far greater than the debates over masks and lockdowns.
Legal scholars suggest that the government does indeed have the legal right to impose mandates for public health reasons – whether the entire population or specific segments (e.g., public employees). Such dictates would, however, likely have unacceptable pushback repercussions.
Businesses will require proof of vaccination before you can use their services. The head of Qantas Airlines has already suggested people would not be allowed to fly without proof of vaccination, for example. Many employers will undoubtedly impose requirements to work as well. We are going to have some complicated months ahead.
With all of this in mind, we can rejoice that there is a light at the end of the tunnel. We have vaccines that work. As we slowly make our transition to a more ‘normal’ society, I urge us to discuss the issues surrounding how we implement COVID vaccines. How we conduct ourselves in the coming months can save countless lives. Regardless, I want to hug my child and enable her to someday describe this nightmarish period to her children and grandchildren as something from the past.
______________________________________________________________________________________________________________________






